People sleeping less than five hours a night have been found to be about 4.5 times more likely to develop a clinical cold than those sleeping more than seven hours.
That is a clue to what sleep really is.
Sleep is not just rest, and it is not simply a way to feel less tired. It changes the condition of the body itself. During sleep, the brain and body shift into a repair-and-regulation state, where immune activity is coordinated, appetite signals are recalibrated, glucose control is restored, memory is processed, stress chemistry settles, and the nervous system gets a chance to downshift.
This is why poor sleep rarely feels like only tiredness. It can show up as cravings, irritability, brain fog, unstable energy, weaker recovery, lower stress tolerance, and the sense that healthy choices require more effort than they should.
This article explains what sleep is actually doing, why rest is not the same thing, and why protecting sleep may be one of the most overlooked foundations of health.
The Strange Risk of Sleep
Sleep is so ordinary that we treat it like breathing, but when you step back, it is one of the strangest states the body enters.
Every night, we become still, less responsive, and partly disconnected from the world around us. We stop eating, working, searching, protecting ourselves, and reacting quickly to danger. For any living creature, that is a vulnerable state.
And yet sleep is so crucial that the body accepts this vulnerable state night after night. That should make us think twice before casually trading it away for another hour of scrolling, gaming, or watching television.
The arrangement does make sleep hard to explain. The body could simply slow down while staying alert. It could conserve energy without making the outside world fade so dramatically into the background, like many animals do.
But that is not what happens.
During sleep, the body enters a different operating mode. Awareness changes. Sensory input is reduced. Muscles relax. The brain cycles through distinct stages. The body becomes less focused on immediate action, like eating and drinking, and more focused on internal regulation and repair.
That does not mean sleep is careless, however. Even during sleep, the brain is not completely absent. A parent may sleep through background noise but wake to the sound of their child. Many people sleep poorly in an unfamiliar place, even when the room is comfortable, as if part of the nervous system is still asking whether it is safe to fully settle.
This is the first clue that sleep is not simple unconsciousness. The sleeping body is vulnerable, but it is not abandoned. It is less responsive, not inactive. It is less outward-facing, not switched off.
So the real mystery is not whether sleep matters. Most people already know that it does. It is why the body has to withdraw from the outside world so deeply in order to do it.
That is where the usual idea of sleep as “rest” begins to fall apart. Sleep is not just a break from life. It is one of the ways life maintains itself.
Sleep Is Not the Body Switching Off
Sleep can look like a shutdown from the outside. The body becomes still. The eyes close. Awareness fades. A sleeping person stops responding to the world with the same speed and precision they have when awake.
But the body is still very much switched on.
But it is a shift into a different biological state. The brain remains active, but its priorities change. Instead of constantly scanning the outside world, planning movement, managing attention, and reacting to immediate demands, it begins cycling through patterns of activity that are more inward-facing.
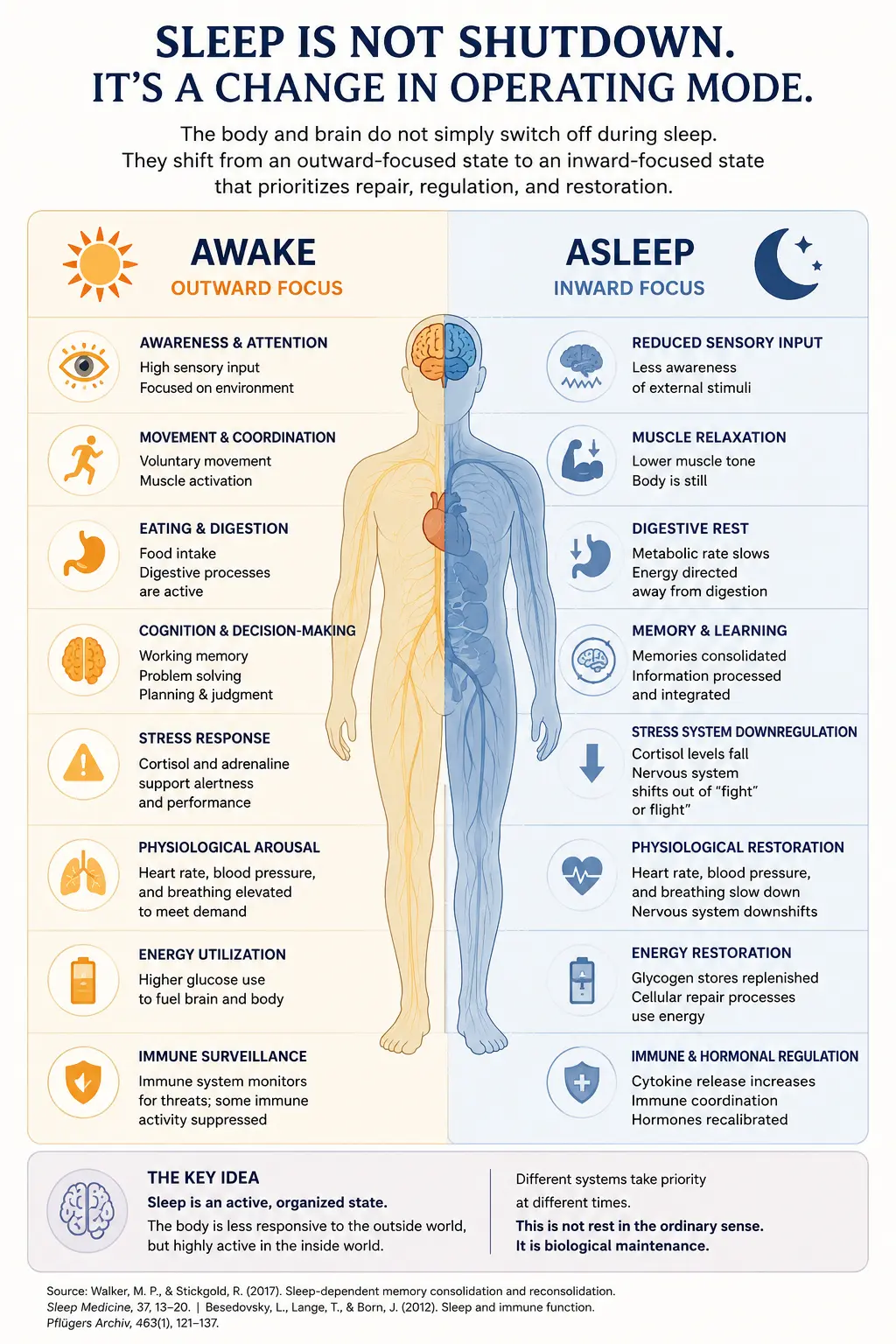
This is why sleep is not the same as unconsciousness. It is not a coma or anesthesia. It is a reversible state where the brain is primed to switch the body back on at a moment’s notice. The sleeping brain is less responsive, but it is still listening. The right sound, touch, discomfort, or sense of danger can bring a person back into waking life.
That distinction changes how we understand sleep. It is not an empty gap of just rest between one day and the next. It is a structured process.
Through the night, the brain moves through different stages of sleep. These stages are not random. They have their own rhythms, patterns, and biological roles. Some parts of sleep are quieter and deeper. Others are surprisingly active, with vivid dreams, emotional processing, and rapid shifts in brain activity.
So while the body may appear still, the system is not idle. Sleep is more like a change in operating mode. Like a supermarket, the lights go down at the front of the building, but work is very much continuing behind the scenes to restock the shelves.
Deep Sleep and REM Sleep
Sleep is usually divided into non-REM sleep and REM (rapid eye movement) sleep.
Non-REM sleep includes the deeper stages of sleep, where brain waves slow down, muscles relax, heart rate and breathing tend to become steadier, and the body becomes harder to wake. This is where sleep most closely matches our idea of physical restoration.
This deep sleep is especially important because it appears to be tied to many of the body’s repair and regulation processes. It is associated with slow-wave brain activity, growth hormone release, tissue repair, metabolic regulation, and the general downshifting of the nervous system after the demands of waking life.
REM sleep, on the other hand, is different. The brain becomes more active again. The eyes move rapidly beneath the eyelids. Dreams are often more vivid, emotional, and story-like. At the same time, most voluntary muscles become temporarily quiet, which helps prevent the body from acting out the dream.

This combination is strange because the brain becomes more active and wake-like, while the body remains mostly still. Brain-wave activity during REM is closer to waking patterns than deep sleep is, which is why REM is sometimes called paradoxical sleep. The person is asleep, but the brain is far from quiet.
REM sleep appears to be involved in memory, emotional processing, learning, and the way the brain integrates experience. But it would be too simplistic to say deep sleep repairs the body and REM sleep repairs the mind, as it is often stated.
Sleep is more integrated than that. Physical health, mental health, memory, hormones, metabolism, and mood are not separate compartments. They are connected systems, and different stages of sleep appear to support them in overlapping ways.
That is why sleep cannot be reduced to just “rest.” Rest is something we can do while awake. We can sit down, close our eyes, relax, and conserve energy.
Sleep goes further.
It changes the state of the brain and body. It alters awareness, hormone patterns, nervous system tone, immune activity, memory processing, appetite signals, and metabolic regulation. It is not simply the absence of activity. It is a different kind of activity — one that waking life cannot fully replace.

Get Your Free Book!
Enter your email to get the free book and occasional updates from The New Health Order.
Nature’s Night Shift
A useful way to think about sleep is as the body’s night shift crew.
During the day, the body is open for business. The brain processes information, muscles contract, glucose moves in and out of cells, hormones respond to stress and food, the immune system monitors threats, and the nervous system stays tuned to the outside world.
That waking state is necessary, but it is not free.
By the end of the day, the body has not simply used energy. It has accumulated work: memories to process, tissues to repair, metabolic signals to rebalance, immune activity to coordinate, and stress chemistry to settle.
Sleep is when the physical inputs stop and the deeper maintenance begins. The brain and body remain highly active, and sleep affects systems ranging from metabolism and immune function to mood, memory, and disease resistance. The National Institute of Neurological Disorders and Stroke describes the sleeping brain and body as “remarkably active,” not switched off.
Sleep also appears to help the brain process experience. A major review in Nature concluded that converging evidence supports sleep as an important period for offline memory reprocessing, helping memories become formed and shaped rather than simply stored.
So the night-crew metaphor is not just poetic. Sleep is when the body shifts away from immediate performance and toward maintenance. It helps regulate the systems that make the next day possible: blood sugar control, appetite, mood, memory, immunity, recovery, and stress tolerance.
That is why poor sleep rarely feels like only one problem.
It can show up as cravings, irritability, brain fog, poor recovery, weaker discipline, worse glucose control, or the vague sense that the body is running behind. Sleep does not merely end the day. It helps the body absorb it, repair from it, and prepare for the next one.
What Sleep Repairs and Regulates
Wakefulness is not free. Every hour we are awake, the body is spending, responding, adapting, and absorbing. The brain processes information. Muscles use fuel. Stress hormones rise and fall. Glucose moves through the bloodstream. Immune cells monitor for damage or threat. Even an ordinary day creates biological work.
Sleep is the daily counterweight to that state.
It does not repair one isolated part of the body because wakefulness does not affect one isolated part of the body. The cost of being awake is spread across the brain, hormones, metabolism, immune system, muscles, and nervous system. Sleep helps bring those systems back into rhythm.
That is why poor sleep rarely feels like one clean symptom. It can show up as hunger, cravings, irritability, brain fog, poor glucose control, weaker recovery, or the sense that the body is running behind. Rest reduces effort. Sleep helps restore regulation.

Hormones, Hunger, and Appetite
One of the clearest places this shows up is appetite.
After poor sleep, many people do not simply feel tired. They feel hungrier, less satisfied, and more drawn toward quick energy. That is not just a willpower problem. Sleep loss can alter the biological systems that help regulate hunger, reward, and food intake.
In this controlled study, for example, 12 healthy young men slept for either eight hours or four hours. After the shorter night, they ate an average of 559 extra calories the next day, about a 22% increase in energy intake. Hunger was also higher before breakfast and dinner.
That does not mean you’re going to automatically overeat after one poor night, but it shows the direction of the problem. Sleep loss can push the body toward eating more, especially in an environment where calorie-dense food is always available.
The usual explanation focuses on leptin and ghrelin, two appetite-related hormones that often work in opposite directions. Leptin, produced largely by fat cells, helps signal energy sufficiency and satiety, while ghrelin, produced mainly in the stomach, tends to stimulate hunger. In the Wisconsin Sleep Cohort, which included 1,024 volunteers, people sleeping five hours had about 15.5% lower leptin and 14.9% higher ghrelin than those sleeping eight hours, alongside a higher BMI.
It must be noted that this hhormone picture is not perfectly settled — some reviews find mixed short-term changes in leptin and ghrelin after sleep deprivation — but the wider pattern is still clear: poor sleep can make appetite harder to regulate. Hunger hormones, reward circuits, fatigue, stress, impulse control, and the modern food environment all interact. A person trying to eat well after a poor night is not working with the same internal conditions as the same person after good sleep.
Glucose and Insulin Sensitivity
Sleep also affects how the body handles glucose.
In a controlled Lancet study, 11 healthy young men were restricted to four hours in bed for six nights. After sleep restriction, their glucose clearance was about 40% slower, their acute insulin response was about 30% lower, evening cortisol was significantly higher, and sympathetic nervous system activity increased. In plain English, even a short period of restricted sleep pushed healthy young men toward poorer glucose handling and a more stressed internal state.
The study was small, so it should not be treated as proof that everyone responds in exactly the same way. But it does show how quickly sleep loss can change the internal conditions that shape metabolism.
This also highlights that the body’s response to food is not fixed. The same meal can be handled differently depending on the state of the person eating it. Sleep, stress, circadian timing, recent movement, liver glycogen, insulin sensitivity, and overall metabolic health all influence how well the body moves glucose out of the bloodstream and into storage or use.
The same healthy intentions can feel very different from one day to the next. Some days cravings are louder, energy crashes come harder, and discipline feels strangely difficult. The food may be the same, but the body receiving it is not.
Immunity and Inflammation
Sleep also helps coordinate the immune system.
A healthy immune system needs rhythm and restraint. It has to respond strongly enough to defend the body, but not so strongly that it creates unnecessary inflammation, overreacts to harmless signals, or stays active when the threat has passed.
Sleep appears to be part of that timing system. A major review on sleep and immune function found that immune activity follows daily rhythms, with certain immune cells and inflammatory signals becoming more active during early nocturnal sleep, while other immune functions are more closely tied to daytime wakefulness. In other words, the immune system is not doing the same thing all day. It is patterned, timed, and influenced by the body’s sleep-wake rhythm.
This becomes more meaningful when we look at infection risk. In one study, 164 healthy adults had their sleep measured for a week before being exposed to rhinovirus under controlled quarantine conditions. Those sleeping less than five hours per night were about 4.5 times more likely to develop a clinical cold than those sleeping more than seven hours.
This is why poor sleep can leave someone feeling run down in a way that is hard to define. It is not only low energy. It may also reflect poorer immune timing, weaker recovery, and less controlled inflammatory signaling.
Inflammation itself is not the enemy—some inflammatory activity is part of defense and repair. The problem is when immune activity loses rhythm, restraint, or proper context, and sleep is one of the daily signals that helps the body know when to defend, when to repair, and when to stand down.
Memory, Mood, and Stress
Sleep also helps the brain process experience.
During the day, the brain absorbs more information than it can fully organize in real time. Conversations, emotions, decisions, learning, stress, conflict, and unfinished concerns all leave an imprint. Sleep gives the brain a different state in which to sort some of that material, strengthen important memories, integrate new information, and regulate the emotional weight of the day.
This is why poor sleep affects more than just recall. It can also affect the quality of the mind the next day.
Poor sleep has been well known to make the brain more emotionally reactive. In one fMRI study, healthy adults kept awake for about 35 hours showed more than a 60% stronger amygdala response to negative images compared with those who slept normally, along with signs of weaker regulation from prefrontal brain regions involved in judgment and emotional control. While the study was small and used total sleep deprivation, not ordinary mild sleep loss, it still helps explain a familiar experience: after poor sleep, small problems can feel larger, stress can feel harder to manage, and self-control can take more effort.
After substandard sleep, small problems feel larger. Irritations feel sharper. Stress feels harder to manage. Food looks more rewarding. Exercise feels harder to start. Conversations require more restraint. The body has not simply lost energy; it has lost some of its regulatory margin.
That is one of the most overlooked effects of poor sleep. It can make health feel like a character problem when it is partly a regulation problem. And from here it’s easy to slip in bad habits and start a slippery slope of bad practices.
While this does not remove responsibility, it should give some helpful context. If someone is repeatedly under-slept, they are trying to make good decisions with a brain that is less prepared to manage appetite, emotion, focus, stress, and impulse control. This is typically not the foundation upon which good decisions are made.
Sleep, then, is not just recovery from tiredness. It is part of how the brain restores control. That is why it sits underneath so many other habits. Nutrition, movement, sunlight, and stress management still matter, but they are easier to use when the body is not fighting the day from a state of poor recovery.
Protect Your Repair System
If sleep is one of the body’s main repair systems, the practical goal is not to treat sleep like an optional luxury. It is to protect the conditions that allow the body to enter that state properly. It should be treated with the same respect and attention as all other facets of health.
The basics still matter most: enough time in bed, consistent sleep and wake times, morning light, daytime movement, darkness at night, sensible caffeine timing, and a calmer transition into the evening. This article here walks through how to improve your sleep environement.
These habits work because they support the body’s timing systems. The body needs clear signals for wakefulness and clear signals for sleep. Modern life often blurs those signals. Bright screens at night, artificial light, late caffeine, alcohol, irregular schedules, constant stimulation, and low daytime movement can all make it harder for the body to know when to be alert and when to repair.
Sleep is where many of the day’s demands are processed. Stress is converted into adaptation. Learning is stabilized into memory. Immune activity is coordinated. Appetite and glucose regulation are brought back toward rhythm. The nervous system gets a chance to downshift.
Poor sleep does not break every system overnight, but it can slowly reduce the body’s ability to regulate itself. That is why it often shows up indirectly: cravings, irritability, brain fog, poor recovery, unstable energy, weaker stress tolerance, and the sense that healthy choices require more effort than they should.
Sleep is not just the end of the day. It is part of how the body prepares for the next one.
So yes, nutrition matters. Movement matters. Sunlight matters. Stress management matters. But sleep helps determine how well the body can use all of them.
That is the real reason sleep matters. Not because it is rest, but because it is repair.
FAQs
1. Why is sleep more than just rest?
Sleep is more than rest because the body does not simply switch off at night. It shifts into a different biological state where the brain and body can process memory, regulate appetite, coordinate immune activity, support glucose control, settle stress chemistry, and recover from the demands of being awake. Rest can reduce effort, but sleep changes the operating state of the whole system.
2. What happens to the body when you do not get enough sleep?
Not getting enough sleep can affect much more than energy. Short sleep has been linked with stronger hunger, higher calorie intake, poorer glucose control, reduced insulin response, greater emotional reactivity, and weaker immune resilience. This is why poor sleep can show up as cravings, irritability, brain fog, unstable energy, poor recovery, and lower stress tolerance.
3. Is deep sleep or REM sleep more important?
Both deep sleep and REM sleep matter, but they appear to emphasize different parts of the repair process. Deep sleep is more associated with slow-wave brain activity, physical restoration, growth hormone release, and nervous system downshifting. REM sleep is more active and dream-rich, and appears to support memory, learning, emotional processing, and experience integration. It is too simplistic to say one matters more than the other; healthy sleep depends on the full cycle.