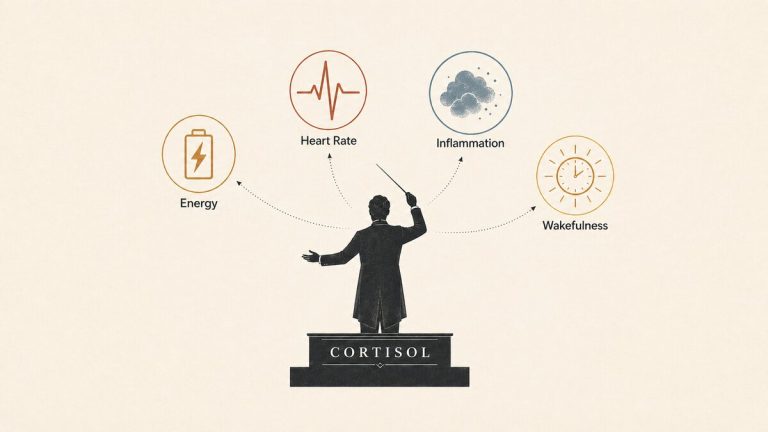
If you have been feeling stressed, tired, wired, or unable to properly switch off, you have probably run into the effects of cortisol. Usually it gets talked about as if it is the problem — the hormone behind anxiety, belly fat, poor sleep, burnout, and feeling generally unwell. But that picture is too simple to be useful.
Cortisol is not just a bad hormone that rises when life goes wrong. It is part of how the body wakes up, stays alert, makes energy available, and responds to challenges. The real issue is not that cortisol exists, or that it ever rises, but when, why, and in what pattern. This article will help you understand what cortisol actually does, why it matters, and when it genuinely starts to become a problem.
Why Cortisol Is So Often Misunderstood
Cortisol is usually introduced with one short label: the stress hormone. While this is not exactly wrong, it often pushes people toward the wrong conclusion. Once cortisol is associated with stress, many people start to hear it as a problem by definition — something the healthy body should try to keep low, quiet, and out of the way.
But stress is not automatically a bad thing. The body is supposed to respond to challenge. It is supposed to wake you up in the morning, sharpen your attention when something matters, make more fuel available during exercise, and help you react quickly in situations that demand it.
Even the classic fight-or-flight response, though often framed negatively, is really a survival system — a way of becoming more alert, responsive, and prepared when the stakes rise. Cortisol is part of that wider response. It rises with stress, but that does not make it something to eliminate. It makes it part of the body’s normal ability to adapt.
The real issue is not simply whether cortisol rises, but when, why, and in what pattern. A rise in the morning is not the same as feeling wired late at night. A temporary increase during exercise is not the same as chronic overload where the body doesn’t get a chance to reset. Most cortisol discussion goes wrong not because it mentions stress, but because it leaves out rhythm, timing, and context.
What Is Cortisol?
Cortisol is a steroid hormone made in the adrenal cortex, the outer part of the adrenal glands that sit on top of the kidneys. It is one of the body’s main glucocorticoids, which means it plays an important role in how the body manages energy, responds to demand, and maintains stability under changing conditions. It helps influence things like blood sugar availability, immune signaling, alertness, and the daily shift between rest and activity.
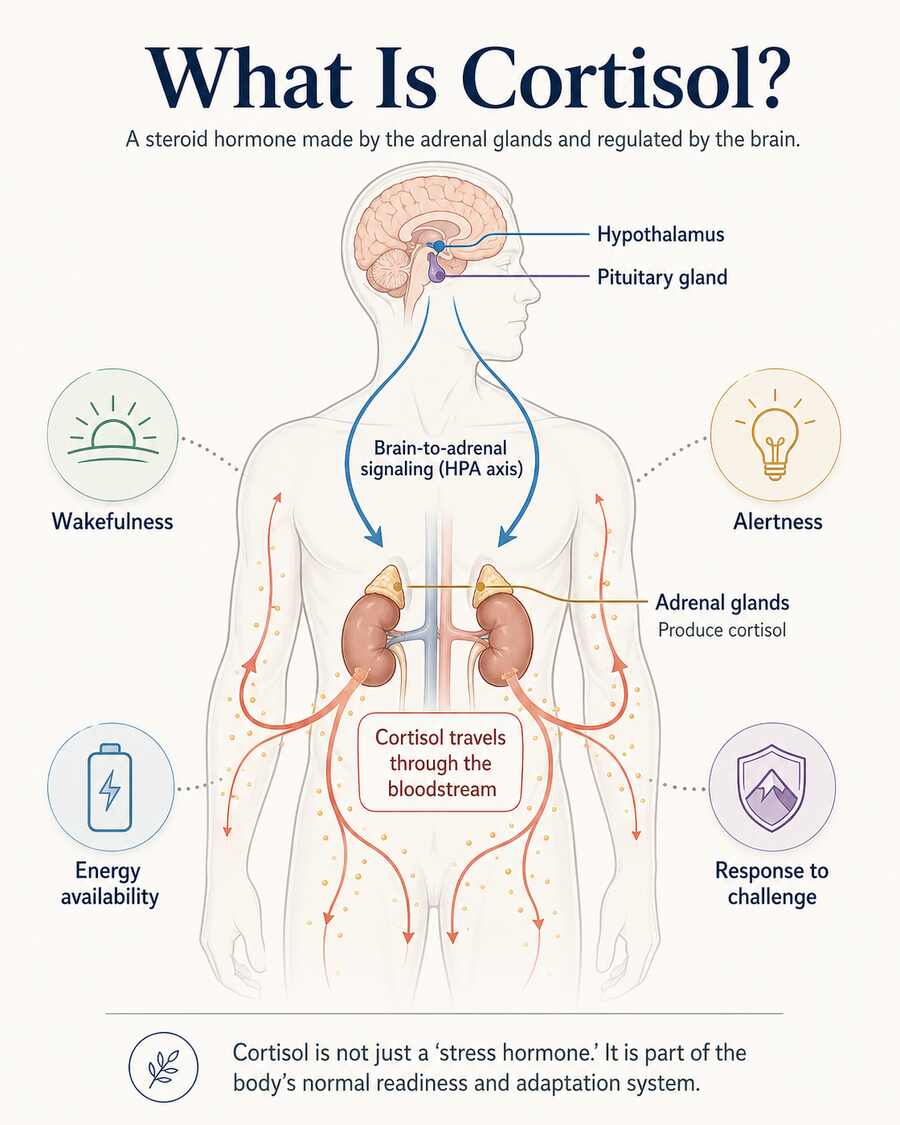
Cortisol is not released at random, and it is not only there for moments of crisis. It is regulated through the HPA axis — a signaling system that links the hypothalamus and pituitary in the brain with the adrenal glands. When the brain detects a need to adjust the body’s state, whether because it is morning, because you are under pressure, because you are exercising, or because you are ill, that system helps coordinate the release of cortisol.
That is why cortisol is better understood as a hormone of adaptation than a sign of damage. It helps the body shift gears. It helps move resources, change priorities, and match physiology to circumstance. The real question is not whether cortisol rises, but whether it is rising in the right rhythm, in the right context, and for the right reasons.

Get Your Free Book!
Enter your email to get the free book and occasional updates from The New Health Order.
What Cortisol Actually Does in the Body
Once you move past the label of “stress hormone,” cortisol starts to make a lot more sense. Its job is not simply to show up when life is going badly. It helps the body adjust to what is happening, both around you and within you. In practice, that means helping you wake up, respond to challenges, and make energy available when it is needed.
Waking Up and Feeling Alert
One of cortisol’s most normal jobs is helping the body transition into wakefulness and daytime readiness. In a healthy rhythm, cortisol usually begins rising in the later part of the night, before you are fully awake, as part of the body’s preparation for the day ahead. In many people, it then rises further in the first part of the morning, helping support alertness, energy availability, and the shift out of the body’s overnight resting state.
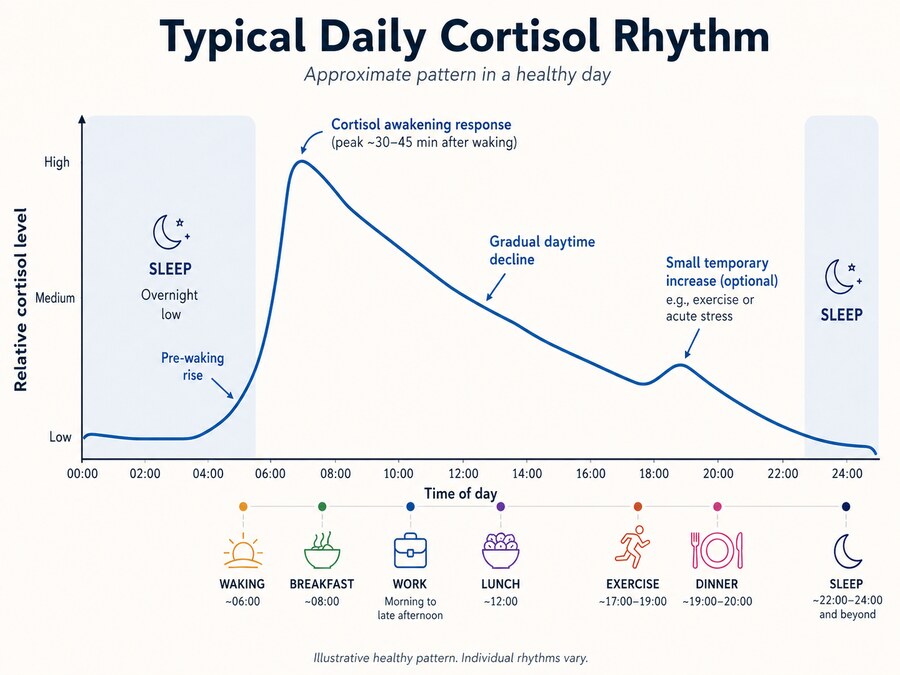
Waking up is not a simple switch from asleep to awake. It is a coordinated biological shift. The body has to move from sleep, repair, and overnight fasting into attention, movement, and daytime function. Cortisol is a vital part of that handover, helping the body become more ready, more responsive, and better able to meet the demands of the day.
There is nothing abnormal about cortisol rising in the morning. That rise is part of how the body gets you moving from sleep into daytime function. The issue is not whether it happens, but whether the pattern still makes sense — whether the body is waking, activating, and settling in a way that feels biologically in step.
Responding to Stress and Challenges
Cortisol also helps the body respond when more is being asked of it. That might mean psychological pressure, like like being under a deadline you feel you cannot miss, but it could just as easily mean exercise, illness, injury, fasting, lack of sleep, or any other situation that forces the body to adapt. In that sense, stress is not always a sign that something is wrong. Often it simply means the body is being challenged, and more resources might be needed to help meet that challenge.
It is also helpful to distinguish cortisol from adrenaline. If you suddenly realise you forgot something important, hear a loud crash, or need to react quickly, that immediate jolt — the racing heart, sharp focus, sudden sense of urgency — is more closely tied to adrenaline and noradrenaline. They are the fast-acting chemicals of alarm and action. Cortisol works more slowly and more broadly. It helps support the response by making fuel available, shifting priorities, and helping the body stay ready if the demand lasts longer than a brief moment.
That is why cortisol should not be thought of as the feeling of panic itself. It is better understood as part of the body’s wider adaptation system. It helps move the body away from rest-and-repair mode and toward a state of greater readiness, where energy, attention, and resources can be directed where they are most needed.
Regulating Energy, Blood Sugar, and Inflammation
Cortisol helps the body manage energy when circumstances change. One of its key jobs is helping make sure enough fuel is available, especially when you have gone without food for a while, are physically active, are under pressure, or are fighting illness. It helps maintain blood sugar partly by supporting gluconeogenesis — the process by which the liver makes new glucose — and by helping mobilise stored energy so the body is less likely to run short when demand rises.
Some tissues, especially the brain, need a steady supply of fuel. The body cannot just drift through the day and hope energy will sort itself out. Between waking, moving, exercising, fasting, thinking, and dealing with stress, supply has to keep being matched to demand. Cortisol is one of the hormones that helps make that adjustment possible. It does not work alone, but it helps shift the body into a state where energy is more available and priorities are reorganised to meet the situation.
Cortisol also plays a role in inflammation and immune signalling; a fact that is often oversimplified. It is true that cortisol can help restrain and regulate inflammatory activity, which is one reason synthetic corticosteroids can be used as anti-inflammatory drugs. But in normal physiology, cortisol is not just there to “turn inflammation off.” It helps shape the immune response, prevent it from becoming excessive, and coordinate how the body responds to injury, infection, or other stressors. In other words, cortisol helps allocate resources not just to energy needs, but to defence and repair as well.
That broader role is what makes cortisol so important. It helps the body decide what matters most in the moment: making fuel available, staying functional, containing inflammation, and getting through the demand in front of you. It is a highly responsive and adaptive hormone that helps ensure your body is prepared for potential challenges.
When Cortisol Becomes a Problem
Cortisol becomes a problem when a system that is meant to help you overcome temporary challenges starts staying switched on for too long, or starts showing up at the wrong times. In a healthy body, cortisol rises and falls with some rhythm and purpose. Trouble starts when that rhythm begins to fray — when stress becomes chronic, recovery is poor, and the body seems less able to settle back into balance.
When Stress Becomes Chronic
The stress response is meant to help you meet a demand and then settle again. That works well when the challenge is brief. It works much less well when the pressure keeps returning, or never really goes away. Poor sleep, financial strain, work stress, caregiving, illness, relationship strain, chronic uncertainty, and constant digital stimulation (endless doomscrolling) can all turn stress into a background condition. In real life, chronic stress usually does not stem from one dramatic emergency, but from being slightly activated too often, for too long, with too little room to fully recover.
That is where the picture starts to change. Cortisol is no longer just helping you respond to something in front of you. It becomes part of a more persistent pattern of strain. Researchers sometimes use the term allostatic load for this — the wear that builds when the systems designed to help you adapt keep getting called on without enough genuine reset. The body is built to handle this and can do it for a while, but it is not meant to live there indefinitely.
One of the clearest places chronic stress shows up is sleep. Stress and sleep tend to feed each other in both directions: when stress stays high, it becomes harder to switch off, and when sleep worsens, stress often feels even less manageable the next day.
This is not just anecdotal. In older adults, frequent chronic stress has been associated with 91% higher odds of difficulty falling asleep, 40% higher odds of waking during the night, and 83% higher odds of waking unrefreshed. Broader survey data point in the same direction: Gallup found that 63% of people who say they need more sleep also report frequent stress, compared with 31% of those who say they get the sleep they need. It this resonates with you, we explored overcoming sleep problems in this article here.
The effects also extend beyond feeling tense or tired. Chronic stress has been linked with broader downstream health problems, including cardiovascular risk. In large meta-analyses, job strain has been associated with about a 20% to 23% higher risk of coronary heart disease— a meaningful increase, especially given how common long-term work stress is.
That, to me, is the real turning point in the cortisol story. The issue is not that the body mounts a stress response, but that a response designed for challenge can slowly become part of the everyday baseline. Once that happens, something useful starts to feel draining.
When Cortisol Rises at the Wrong Time
Cortisol is supposed to help you get going, not keep you half-switched on all night. In a healthy rhythm, it is higher when the body needs to be awake, alert, and ready, and lower when the day is winding down. When that timing starts to slip, things can feel off even if nothing dramatic is happening.
This is where the familiar tired-but-wired feeling often lives. You can feel drained, but still strangely unable to let go of the day. Sleep feels delayed, shallow, or less restorative. The body is tired, but not fully getting the message that it is safe to power down. Hours of mindless tossing and turning in bed often follows, as you are tired but unable to switch off. That is what mistimed activation does. It keeps nudging physiology in the wrong direction.
The body is supposed to do something different at night than it does during the day. Night should favour slowing down, letting go of alertness, and shifting more fully into rest and recovery. When cortisol keeps nudging the system toward wakefulness instead, the problem is not just a rough night. Over time, it can begin to throw the wider rhythm out of step.
When the Daily Pattern Loses Its Shape
The deeper issue is often not one stressful moment, or even one bad night. It is a daily pattern that no longer feels clean and well timed. In healthy physiology, cortisol tends to follow a recognisable shape: it rises to help you wake up and meet the day, then gradually falls as the body moves toward evening and rest. That curve does not need to be perfect, but it does need some overall rhythm.
When that rhythm starts to flatten, drift later, stay too elevated into the evening, or vary too much from day to day, the system can start to feel less steady. The body may feel harder to wake, harder to calm, or less able to move cleanly between effort and recovery. This is one reason broad phrases like “high cortisol” are often too simplistic. What matters is not just whether cortisol is elevated, but whether the overall pattern still makes biological sense.
Normal vs Problematic Cortisol Patterns
| Pattern | More likely normal / adaptive | More likely problematic |
| Morning cortisol | Rises around waking, helps alertness | Hard to wake, flattened morning response |
| Daytime stress response | Temporary rise with exercise, illness, challenge | Feels constantly activated, never fully settles |
| Evening cortisol | Falls as body winds down | Tired but wired, harder to switch off |
| Overall rhythm | Clear rise-and-fall across the day | Flattened, delayed, inconsistent, or elevated too late |
Final Thoughts – How to Think About Cortisol Properly
Cortisol is not best understood as a problem to eliminate. It is better understood as part of the body’s normal readiness system — a hormone involved in waking, adapting, mobilising energy, and helping you cope with demand.
What matters most is not whether cortisol rises, but whether the overall pattern makes sense. A healthy body should be able to rise to a challenge and then settle again. Trouble starts when stress becomes too constant, recovery too limited, and the rhythm between activation and rest begins to break down.
So the practical takeaway is simple: stop asking only how to lower cortisol, and start asking what your body is responding to. Sleep, light, pressure, illness, workload, under-recovery, circadian disruption, and overall life strain all matter. Cortisol is not the whole story. But it can be a very useful clue to whether the story your body is living in still makes biological sense.
FAQs
Is cortisol good or bad?
Cortisol is not inherently bad. It is an essential hormone that helps regulate wakefulness, energy availability, inflammation, and the body’s response to stress. Problems usually come from chronic or mistimed patterns, not from cortisol existing or rising at all.
What does cortisol do in the body?
Cortisol helps the body wake up, stay alert, make glucose available for energy, regulate aspects of inflammation and immune signalling, and respond to physical or psychological stress. It is produced by the adrenal glands and is part of the body’s wider adaptation system.
When is cortisol a problem?
Cortisol becomes more problematic when the stress response becomes chronic, when cortisol stays elevated or shows up at the wrong time of day, or when the normal daily rhythm starts to lose its shape. True endocrine disorders such as Cushing syndrome or adrenal insufficiency are different from vague internet self-diagnosis.