If you have ever felt exhausted but still unable to fall asleep, cortisol may be part of the reason. It is often blamed as a “stress hormone,” but that label is too blunt to explain what is really going on. Cortisol helps regulate wakefulness, alertness, and the body’s daily rhythm, which means sleep can start to suffer when that pattern becomes strained, mistimed, or too slow to settle.
That is what makes sleep problems so confusing. You can feel tired enough to want sleep badly, yet still not feel properly ready for it. This article will explain how cortisol fits into the sleep-wake cycle, why people can feel tired but still too switched on to rest, what pushes cortisol in the wrong direction at night, and what tends to help when the body feels too alert to sleep.
What is Cortisol?
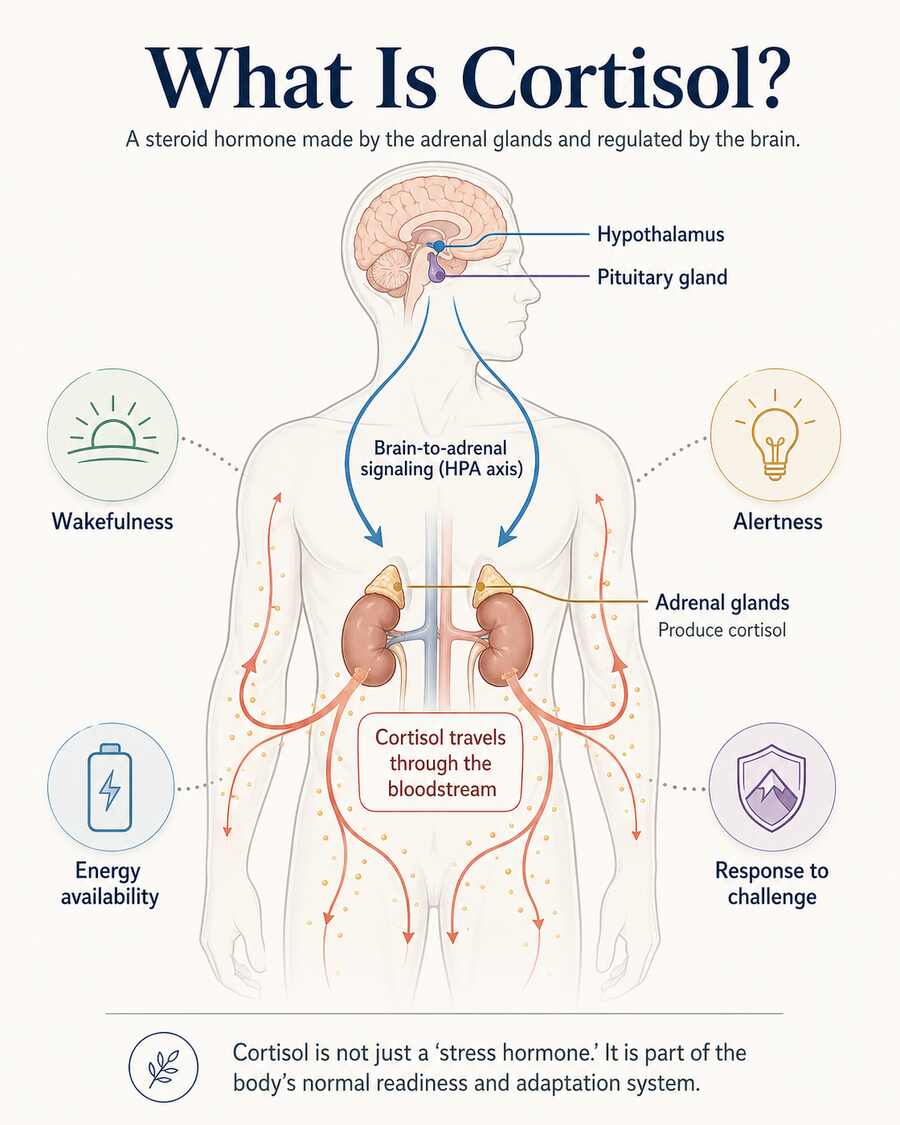
Cortisol is a steroid hormone made by the adrenal glands. Because it is made from cholesterol, it can act inside cells and help shape how the body manages energy, inflammation, and stress. More broadly, cortisol is part of the body’s adaptation system — one of the hormones that helps you respond when circumstances change.
That is why cortisol reaches into so many parts of daily life. It helps regulate wakefulness, energy availability, immune and inflammatory signalling, and the body’s response to challenge. It is often introduced as “the stress hormone,” but that label only captures part of the picture.
What makes cortisol especially relevant to sleep is that it follows a daily rhythm. In a healthy pattern, it stays lower through the night, then rises toward morning to help bring the body into wakefulness before gradually falling again later in the day. So cortisol is not just about stress in the emotional sense. It is part of the body’s wider timing system as well. For a fuller explanation of what cortisol is and what it does in the body, see What Does Cortisol Do?
Why Cortisol Matters for Sleep
Sleep is not controlled by one chemical alone. It depends on a balance between sleep pressure, circadian timing, and the body’s level of alertness. Adenosine, a molecule derived from ATP, helps build sleep pressure the longer you stay awake. The hormone melatonin helps signal darkness and biological night. Cortisol belongs to the other side of the equation. It is part of the body’s readiness system, helping shape when you feel more alert, more awake, and more prepared to meet the day.
In a healthy rhythm, these signals work together to optimize sleep quality. As the day goes on, adenosine gradually builds, creating more pressure to sleep (coffee works by temporary blocking adenosine). Later in the evening, melatonin begins to rise, helping tell the body that night has arrived.
Cortisol generally does the opposite. It stays lower through the night, then begins to rise toward morning as the body prepares to move back into wakefulness. Sleep tends to come more easily when those signals are aligned — when sleep pressure is building, melatonin is rising, and cortisol is no longer pushing too hard in the direction of alertness.
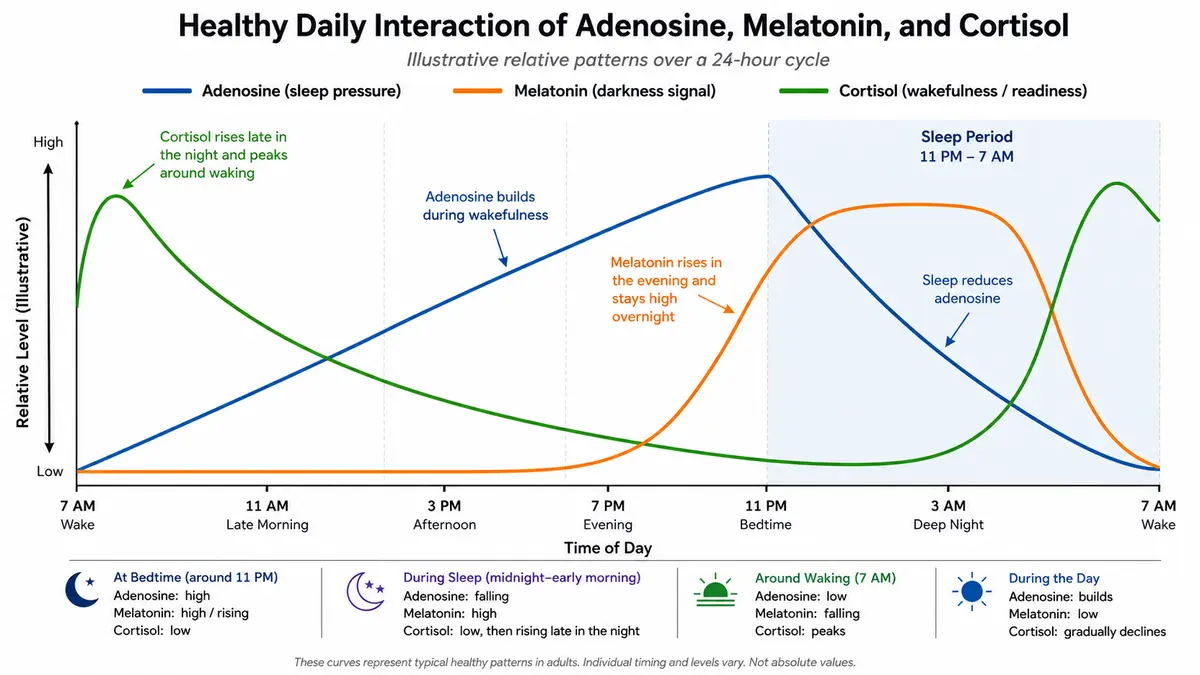
This is one reason people can feel tired but still not properly ready for sleep. The issue is not always a lack of sleepiness, but a body that is still leaning too far toward alertness. You may have enough adenosine on board to feel exhausted, and melatonin may be rising as it should, but if cortisol remains elevated or shows up at the wrong time, sleep can feel harder to enter and harder to stay in.
It is also worth remembering that cortisol is not there only to regulate the sleep-wake cycle. It can rise in response to psychological stress, illness, exercise, pain, fasting, and other demands on the body. That is part of why sleep can become so easily disrupted. Cortisol is involved in normal wakefulness, but it is also part of the body’s broader adaptation system, which means that what is happening in the rest of your life can spill into the night as well.
Cortisol’s Main Roles in the Body
| Role of cortisol | Why it matters |
| Wakefulness | Helps the body transition into alertness and daytime readiness |
| Stress response | Helps the body respond when more is being asked of it |
| Energy and blood sugar | Helps keep fuel available when demand rises |
| Inflammation and immunity | Helps regulate and shape the body’s response to injury, infection, and stress |
| Circadian rhythm | Follows a daily pattern that helps separate day from night |
| Adaptation | Helps the body shift priorities depending on what is happening |

Get Your Free Book!
Enter your email to get the free book and occasional updates from The New Health Order.
Why You Can Feel Exhausted but Still Too Alert to Sleep
One of the strangest parts of poor sleep is that tiredness and sleepiness are not always the same thing. You can feel worn out, mentally foggy, and desperate for rest, yet still not be in a state that allows sleep to come easily. Anyone who has lain in bed exhausted but restless, unable to properly switch off, will recognise that strange mix of frustration and confusion. It feels as though sleep should simply happen once you are tired enough. But the body does not always work that way.
For sleep to come naturally, it is not enough to have built up sleep pressure. The body also has to let go of alertness. It has to shift out of problem-solving mode, out of vigilance, out of that slightly braced state that keeps you half-ready for whatever comes next. When that shift does not happen cleanly, you can end up in the familiar tired-but-wired state: heavy, drained, and clearly in need of sleep, but still too switched on to fully drop into it.
This is where cortisol becomes relevant. Not because it is the only thing involved, and not because every bad night means you have a cortisol problem, but because cortisol is part of the wider physiology of readiness. Research does support a link between poor sleep and altered cortisol rhythms.
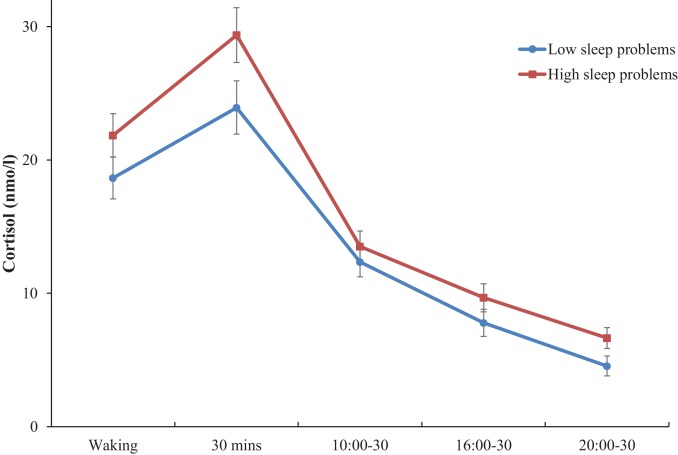
A 2022 meta-analysis found that people with chronic insomnia had a moderately more activated cortisol profile than people without insomnia. The difference was large enough to suggest a real pattern, not just random noise, but not so large that every person with insomnia would show obviously extreme cortisol levels.
Another study found that longer sleep latency (taking longer to fall asleep) was associated with a 30.4% blunting of the normal cortisol awakening rise the next morning. Poor sleep and disrupted cortisol patterns do seem to go together, even if the problem is usually one of timing and rhythm rather than simply “high cortisol.”
That is why people can lie in bed feeling utterly spent and still not settle. The issue is not always that they are not tired enough. Sometimes it is that the body has not fully released the day. Sleep pressure may be there, but the internal conditions for sleep are still incomplete. When the system is still leaning too far toward alertness, sleep can start to feel blocked by something harder to name than simple stress. The body may be tired, but it is not fully acting like night has arrived.
When Cortisol and Sleep Start to Work Against Each Other
At first, cortisol and sleep are part of the same system. One helps pull the body toward wakefulness, the other depends on the body being able to let go of that wakefulness at the right time.
The trouble starts when that handover stops happening cleanly. Instead of rising and falling with some rhythm, cortisol begins to reflect a body that is under too much strain, too poorly timed, or too slow to settle. That is when a useful stress system can start working against the very recovery the body needs.
Chronic Stress Can Keep the Body Too Alert
The stress response is meant to help you meet a challenge and then ease off. But chronic stress does not behave like one short challenge. It can come from work pressure, relationship strain, illness, poor sleep, financial worry, caregiving, or any other myriad problems. When that happens, the body can stay in a more activated state than it was designed to sustain, and sleep is often one of the first places that shows up.
Biologically, this is often described as hyperarousal. The person may feel tired, but the body is still leaning too far toward vigilance. Research supports that picture. In studies of insomnia, both ACTH (the brain’s signal telling the adrenal glands to make cortisol) and cortisol itself can remain elevated across the 24-hour day. That suggests the problem is not just a lack of sleepiness, but a stress-alertness system that is staying more activated than it should.
A 2019 study adds another useful layer to this. Among people with insomnia, those showing signs of hyperarousal had higher urinary cortisol across the day than those without hyperarousal, suggesting that some sleep problems are happening in a body that is still running too alertly, not in one that has fully shifted into a night-time state.
That helps explain why chronic stress and poor sleep so often feed each other. The more activated the body remains, the harder it becomes to enter deep, restorative sleep. And the less restorative sleep you get, the harder it becomes to regulate stress cleanly the next day. What starts as a response to pressure can slowly become part of the everyday baseline.
Mistimed Cortisol Can Delay Sleep and Disrupt Recovery
Cortisol does not only cause problems when there is too much of it. It can also cause problems when it shows up at the wrong time. In a healthy rhythm, cortisol is relatively low in the evening and overnight, then begins rising toward morning to help the body move into wakefulness. When that pattern drifts later, stays elevated into the evening, or becomes flatter across the day, sleep tends to suffer because the body is still receiving a signal that leans toward alertness instead of rest.
There is real data behind this. A 2021 review found that six studies reported higher afternoon or evening cortisol when sleep opportunity was reduced to 5.5 hours a night or less. One of the classic studies in that literature found that after partial and total sleep deprivation, cortisol levels between 6 p.m. and 11 p.m. were 37% and 45% higher, respectively, than the previous day.
Once that mistiming becomes a pattern, recovery can start to suffer in a wider sense. Sleep is when the body shifts more fully toward repair, immune regulation, energy restoration, and the unwinding of daytime activation. If cortisol keeps nudging the system back toward wakefulness instead, even subtly, sleep can become lighter, more delayed, or less restorative. Over time, that makes it harder for the body to separate day from night in the clean way healthy physiology depends on.
What Pushes Cortisol in the Wrong Direction at Night
Night-time cortisol does not usually rise in a vacuum. More often, it is being pulled there by something. Sometimes that is psychological stress and unresolved mental load. Sometimes it is a mistimed light environment, an irregular sleep schedule, late caffeine, pain, illness, or a body that no longer gets clean enough signals for when day ends and night begins.
Cortisol matters here because it is part of the body’s wider alertness system. When enough things keep pushing the body toward vigilance and wakefulness, sleep can start to feel less natural and more like something the system is resisting.
Psychological Stress and Mental Load
This is probably the most familiar driver, and also one of the most common. Gallup reported in 2024 that 49% of Americans say they frequently experience stress, and among those who say they need more sleep, 63% also report frequent stress, compared with 31% of those who say they get the sleep they need.
APA’s 2024 Stress in America data point in the same direction: 77% of adults said the future of the nation was a significant source of stress in their lives, and 73% said the same about the economy. In other words, many people are not arriving at bedtime from anything like a calm baseline. They are arriving there already carrying a meaningful background load.
The significance here is that stress at night is not always dramatic—often it is quieter and more subtle than that. It can look like replaying a conversation, thinking through tomorrow, feeling financially stretched, carrying family worries, or lying in bed with the vague sense that something is still unresolved.
This is where rumination and overthinking can become more than a mental nuisance; they can keep the body acting as though the day is not finished.
Insomnia research often describes this in terms of sleep reactivity or hyperarousal — the idea that some people’s sleep is especially easy to disrupt when stress rises. The problem is not just that they are “thinking too much.” It is that the whole system is staying more alert than sleep requires.
Cortisol is not the only thing involved in that state, but it is part of what helps sustain it. If the brain is still acting as though more readiness is needed, cortisol can help keep energy available and the body slightly braced, even when the person consciously wants to sleep. That is one reason mental load matters so much. The mind may still be working on the day, and the body ends up following it into the night.
Light, Sleep Timing, and Circadian Disruption
Not all night-time activation comes from feeling stressed. Sometimes the body is simply getting mixed signals about whether it is still daytime. Light is one of the strongest cues the circadian system uses to organise the sleep-wake cycle, which is why bright light in the evening, irregular sleep timing, or frequent shifts in schedule can make it harder for the body to move cleanly into night mode. Reviews of the field show that evening light can delay circadian timing, suppress melatonin, and increase alertness at the very time the system should be winding down.
healthy pattern, cortisol stays relatively low in the evening and rises toward morning as wakefulness approaches. When circadian timing drifts later, that pattern can drift with it. The result is not always dramatic, but it can be enough to make the body feel less ready for sleep and less able to separate day physiology from night physiology. Night shift workers often run straight into this problem, because the body is being asked to stay alert and work at a time it would normally be moving toward rest, then sleep at a time it would normally be preparing for wakefulness.
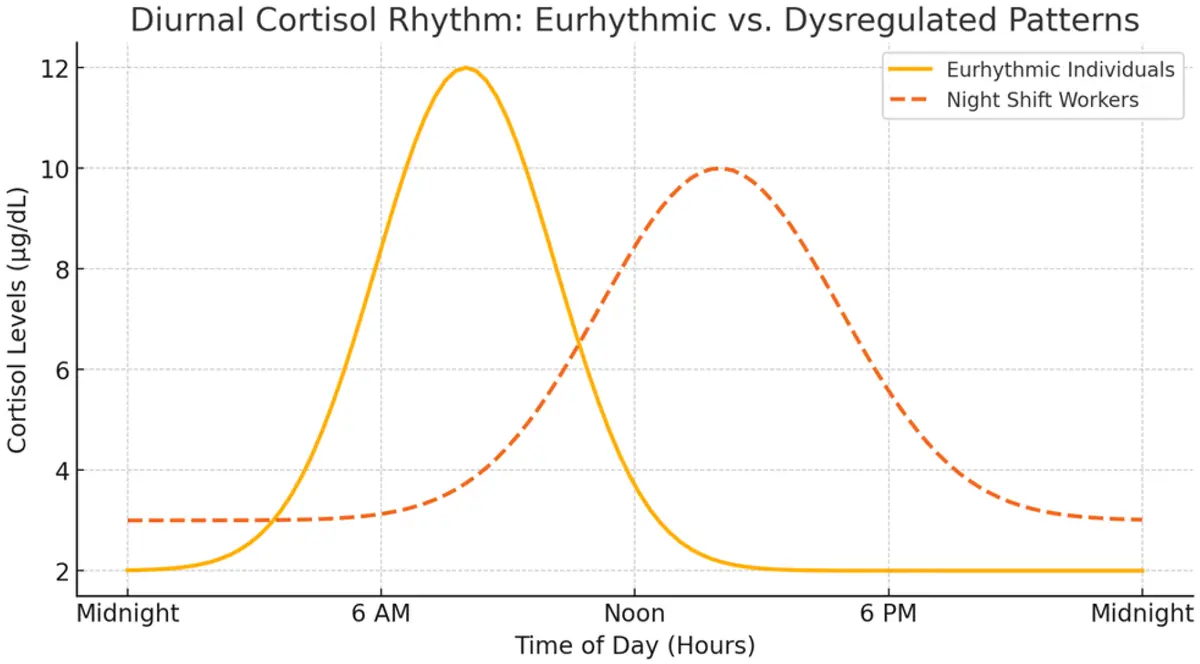
Sleep loss can make this even messier. Experimental work suggests that substantial sleep restriction and circadian misalignment can raise cortisol later in the day, especially in the late afternoon and early evening, which is exactly when the system should be easing away from alertness. So someone can end up in a loop where late nights, bright evenings, and irregular timing all keep nudging the body in the wrong direction.
Caffeine, Illness, Pain, and Other Sources of Night-Time Activation
Some night-time activation is less psychological and more mechanical. Caffeine is a good example. In healthy adults, the mean half-life of caffeine is about 5 hours, but the range is wide, roughly 1.5 to 9.5 hours, which means it can stay in the body much longer than people expect.
A simple example makes the point: an average 8-ounce cup of brewed coffee contains about 95 mg of caffeine. If someone drinks that at 4 p.m., they may still have roughly 47 mg in their system at 9 p.m. and around 24 mg at 2 a.m. if they clear caffeine at an average rate. For some people, especially those who are more sensitive to caffeine, that may still be enough to interfere with sleep.
While caffeine is great for waking us up or giving us that post lunch boost, research shows it can meaningfully worsen sleep. Reviews have reported that evening caffeine can reduce total sleep time by about 45 minutes, lower sleep efficiency by around 7%, increase the time it takes to fall asleep by about 9 minutes, and increase time awake after sleep onset by roughly 12 minutes. So someone can feel tired, genuinely want to sleep, and still have enough caffeine on board to keep the body leaning the wrong way.
Pain and illness can do something similar. Pain is strongly linked with poor sleep in both directions: pain disrupts sleep, and poor sleep increases next-day pain sensitivity. Illness can also keep the body more activated than restful, especially when inflammation, discomfort, congestion, or recovery demands are in the background.
In those situations, the problem is not always “stress” in the narrow psychological sense. Sometimes the body is simply not comfortable, settled, or well enough to move cleanly into a deeper night-time state.
What Helps When the Body Feels Too Alert to Sleep
When the body feels too alert for sleep, the goal is not to force cortisol down. It is to reduce unnecessary activation and make the day-night pattern clearer again. In practice, that usually means lowering the inputs that keep the system switched on and strengthening the cues that tell the body when it is time to wind down.
Reducing Night-Time Activation
Some sleep problems are made worse because the body is still being pushed toward alertness late in the day. The most common examples are:
- Late caffeine: the buzz may be gone, but the caffeine may not be. A late coffee can still be active in the system by bedtime.
- Mental load: unfinished work, financial stress, family pressure, and rumination can all keep the system half-switched on.
- Late stimulation: work, intense exercise, arguments, news, and endless scrolling can all make it harder to shift into a quieter state.
- Pain or illness: discomfort, inflammation, congestion, and general unwellness can keep the body more vigilant than restful.
- Trying too hard to sleep: once bedtime becomes associated with frustration or pressure, the bed itself can become part of the problem.
The deeper point that connects all of these together is that when the body still feels as though something is happening, it may stay more alert than sleep requires.
Strengthening the Signals for Day and Night
The other side of the equation is helping the body tell day from night more clearly. That usually means:
- Get light earlier in the day: morning light helps reinforce the body’s sense that daytime has started.
- Keep wake time fairly consistent: regular waking tends to stabilise the wider rhythm more than focusing only on bedtime.
- Reduce bright light late at night: especially overhead light and screens used close to bed.
- Let evening feel more like evening: lower stimulation, less mental input, and a clearer sense that the day is ending.
- Avoid constantly shifting your schedule: irregular sleep timing can make the body less certain when it should be alert and when it should be winding down.
When the Problem Is Ongoing Stress
Sometimes the problem is not really poor sleep habits. It is that life itself is keeping the system too activated to settle properly. Chronic work pressure, relationship strain, caregiving, grief, anxiety, or constant uncertainty can all leave the body arriving at bedtime already carrying too much load. Over time, that load can also spill into appetite, cravings, blood sugar, and fat storage, which is why stress and poor sleep often show up far beyond bedtime.
In that situation, darker lights and less caffeine may still help, but they may not be enough on their own. If the sleep problem has become chronic, CBT-I (Cognitive Behavioral Therapy for Insomnia) is often the most evidence-based place to start. If the body seems stuck in stress, anxiety, rumination, or emotional overload, it may also be worth looking into support from a psychologist or therapist, because the issue may be bigger than sleep itself.
Final Thoughts – How to Think About Cortisol and Sleep Properly
Cortisol is not best understood as a sleep problem in itself. It is better understood as part of the body’s normal readiness system — a hormone involved in wakefulness, adaptation, and the shift between rest and alertness.
That is why it matters so much for sleep. In a healthy pattern, cortisol helps support wakefulness at the right time and then eases back as the body moves toward night. Trouble starts when that rhythm becomes chronically strained, mistimed, or too slow to settle.
So the practical takeaway is not to fear cortisol, and not to assume the answer is simply to “lower it.” The more useful question is what the body is responding to. Sometimes that means stress, mental load, poor recovery, circadian disruption, late caffeine, pain, illness, or a day that never really got put down. Sleep often improves not when one hormone is attacked in isolation, but when the wider pattern starts to make more sense again.
It is also worth keeping some perspective. Not every bad night, and not every stretch of poor sleep, is mainly a cortisol problem. Sleep apnea, pain, restless legs, medication effects, mood disorders, illness, and other sleep disruptions can all matter too. Cortisol is one part of the picture, not the whole picture.
The best way to think about cortisol and sleep, then, is not in black and white. It is not “cortisol bad, sleep good.” It is a question of pattern. Is the body able to rise when it needs to rise, and let go when it needs to let go? When that rhythm is working, sleep comes more naturally. When it is not, cortisol can be a useful clue — not because it explains everything, but because it tells you something important about the state your body is still stuck in.
FAQs
Can cortisol cause sleep problems?
Cortisol can contribute to sleep problems when it stays elevated too late, rises at the wrong time, or becomes part of a broader pattern of chronic stress and hyperarousal. The issue is usually one of timing and rhythm, not simply “high cortisol.”
Why do I feel tired but wired at night?
You can feel tired but wired when sleep pressure is there, but the body is still leaning too far toward alertness. Stress, late caffeine, pain, light at night, and circadian disruption can all make it harder to fully switch into a night-time state.
Is cortisol always the reason for poor sleep?
No. Cortisol can be part of the picture, but poor sleep can also be driven by sleep apnea, pain, illness, medication effects, restless legs, anxiety, depression, or an irregular sleep schedule. Cortisol is one possible factor, not the whole explanation.