A lot of people believe they’re stuck with a “slow metabolism”—that some people are simply born burning fewer calories, and that’s why fat loss feels impossible for them. This is simply not the case.
In reality, metabolism isn’t a fixed trait. It’s a responsive system that adjusts to what you repeatedly do: what you eat, how often you eat, how much demand you place on your muscles, how you sleep, and the stress signals your body is living under.
Fat is also more complex than most people realise. It isn’t just “extra weight.” It’s a regulated energy reserve that your body actively manages, using hormones and fuel-routing decisions that change hour by hour. And when you don’t understand the system, it’s easy to assume your body is working against you.
This article breaks down the biology of fat storage and fat use in plain language. You’ll learn where incoming energy can go (burned now, stored as glycogen, stored as fat), how hormones like insulin and stress signals influence storage and release, why you can still burn fat even while eating carbs, and why modern patterns—ultra-processed foods, frequent snacking, poor sleep, high stress, and low activity—make fat gain so common. You’ll also see why fat loss often stalls and what to focus on to make it easier, without gimmicks or extreme rules.
If you’ve been blaming your metabolism, this will give you a clearer framework: not motivation, not magic—just a practical understanding of how to get your metabolism working in your favour.
Why Does the Body Store Fat?
Body fat isn’t a mistake. It’s a normal tissue with a clear purpose: storing energy and helping regulate how your body uses fuel. When you understand what it’s doing, fat gain and fat loss become much easier to interpret and manage.
Fat as Long-Term Energy Storage
At its most basic, body fat exists for one reason: to store energy for later. Your body has ongoing energy costs—brain function, body temperature, tissue repair, immune function—whether you ate today or not. In the modern world, we treat food like it’s guaranteed, but your biology was built in a world where it wasn’t.
That’s why the body uses two main storage systems:
- Glycogen (stored glucose, mostly from carbohydrates but sometimes from protein in small amounts) is short-term storage. Stored in the liver and in muscle tissue, it’s useful, fast-access fuel, but capacity is limited.
- Body fat is long-term storage. It’s energy-dense, stable, and scalable—meaning you can store a lot of it without needing a huge amount of space or water.
That “energy-dense” part matters immensely, and is true for most mammals across the animal kingdom. Fat is the most efficient way to store surplus energy in the body. It’s essentially the body’s way of saying: if energy is available now, it’s smart to bank some for later.
Glycogen vs Body Fat: Your Two Energy Stores
| Feature | Glycogen (stored glucose) | Body fat (stored triglyceride) |
| Main role | Short-term backup fuel | Long-term energy reserve |
| Where stored | Liver and muscles | Adipose tissue (fat cells) |
| Capacity | Limited | Large / scalable |
| Speed of access | Very fast | Fast, but more regulated |
| Energy density | Lower (and stored with water) | Very high (compact) |
| Typical use | Between meals, exercise, overnight glucose support | Longer gaps, sustained energy needs |
See this article here for a in-depth look at glucose vs. fat as different fuels.
Other Roles: Hormones, Insulation, Protection
A lot of people think of fat tissue just as a passive “storage bin,” but adipose tissue (commonly known as body fat) is active. It’s involved in multiple functions beyond energy storage:
- Hormone signaling: Fat tissue produces signaling molecules (like leptin) that help the brain regulate hunger, metabolism, and energy availability. In simple terms, fat stores are part of the body’s “fuel gauge.”
- Insulation and temperature regulation: Especially in colder environments, body fat helps reduce heat loss.
- Physical protection: Fat provides cushioning around organs and helps protect tissues from mechanical stress.
So even before we talk about weight loss, it helps to recognize that fat isn’t a mistake the body makes—it’s a tissue the body uses for multiple survival purposes.
When Fat Storage Increases Beyond Normal
The next question is the one people are mostly concerned about: if fat storage is normal, why does it sometimes increase to a level that becomes unhealthy or stubborn?
In general, fat storage rises when the body repeatedly receives a combination of signals that make storage the safe option:
- More energy coming in than being used over time
This is the non-negotiable backdrop. If energy intake persistently exceeds energy demand (commonly known as calories in vs. calories out, although there’s a little more to this in reality), the body has to store the excess somewhere. And once glycogen stores are full and there’s no other place for glucose to go, fat is the only remaining option. - Low demand for stored fuel
If muscle glycogen isn’t being depleted regularly (low movement, little resistance training), the body has less reason to keep a large “ready-to-burn” fuel turnover in the liver and in muscle tissue. Fat storage becomes more likely because the glycogen storage system is underused. - Hormonal and appetite signals that keep the body in “store and defend” mode
Insulin is one of the main culprits of fat storage signals as it moves incoming nutrients into storage and reduces fat release while elevated—but it’s not the only signal. Sleep loss, chronic stress, and highly rewarding processed foods can all shift hunger and satiety regulation, making it easier to overconsume and harder to access stored energy comfortably. (See this article here for an in-depth look at one of the most powerful hormones in the body – insulin – and how it relates to fat release.) - Reduced metabolic flexibility (common in insulin resistance)
When the body struggles to switch smoothly between burning glucose and burning fat (known as metabolic inflexibility), people often experience stronger hunger swings and less stable energy, which nudges them toward more frequent eating and less reliance on stored fuel. That doesn’t create energy out of nowhere—it changes the conditions that make fat storage more likely and fat loss harder to sustain.
The key takeaway here: fat storage isn’t random. It’s the predictable result of a storage system responding to energy availability, demand, and internal signals.

How Does the Body Decide to Store vs Burn Fat?
Your body is not broken or not working optimally when it stores fat. It’s also not storing fat because you have genetically poorer “metabolism”.
Your body is way more sophisticated than that. It’s making a series of very clever fuel-management decisions based on two simple things: what energy is coming in, and what energy is being demanded right now. Most of the confusion around fat loss comes from people imagining the body is either “in fat-burning mode” or “in fat-storing mode” permanently. In reality, it moves between the two all day, and it’s supposed to.
Where Incoming Energy Can Go
Every meal delivers energy mainly as glucose (from carbohydrates, and some from protein indirectly) and fatty acids (from dietary fat, and also from stored body fat when it’s released). Once those fuels enter the bloodstream, the body has three basic options:
- Burn it now for immediate energy.
If you’re active, stressed, thinking hard, or simply maintaining basic body functions, a portion of incoming fuel is oxidized and used right away. - Store it short-term as glycogen (stored glucose).
After the body has burned all it needs to for immediate use, glucose can be stored in the liver and muscles as glycogen. This is useful because it provides quick-access fuel, especially for higher-intensity work. - Store it long-term as fat (in adipose tissue).
When energy coming in exceeds what can be used immediately or stored as glycogen, the body then begins to store the remainder primarily as triglycerides in fat tissue.
The reason the body prioritizes glucose isn’t because it’s a “better” fuel, as many mainstream outlets will tell you—it’s because high blood glucose is harmful if it stays elevated. Glucose in the bloodstream must be tightly regulated, so insulin acts quickly to move it into tissues and bring levels back down. This is also why insulin resistance and diabetes matter: when glucose stays high for longer, it increases cellular stress and long-term damage risk.
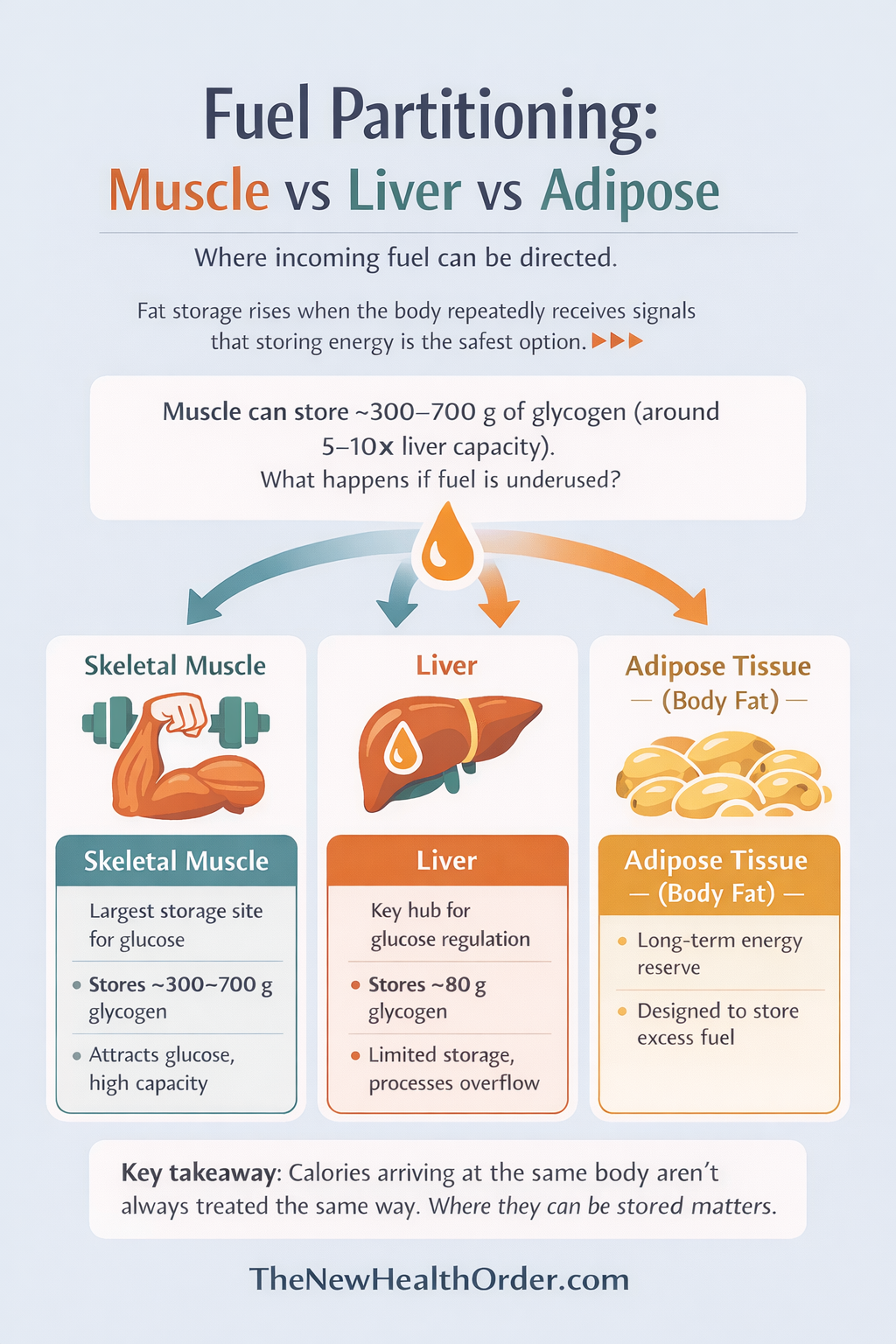
Fuel partitioning: Muscle vs Liver vs Adipose
The next layer is where that incoming fuel gets sent. This is called fuel partitioning, and it’s one of the most overlooked parts of the story because it explains real-world differences between people’s different weight loss journeys.
Skeletal muscle is the body’s largest storage site for glucose. Depending on muscle mass and training status, muscle glycogen stores are often estimated around 300–700 g, compared with a much smaller liver glycogen reserve.
After exercise—especially when glycogen has been depleted—muscle becomes a stronger sink for incoming carbohydrate, and the size of this effect tracks with how much glycogen you emptied. Post-exercise, the body can direct a surprisingly large amount of carbohydrate toward refilling glycogen—often on the order of ~1.0–1.2 g/kg/hour in the early recovery window
The liver is another key hub. It stores some glycogen (around 80g), helps regulate blood sugar between meals, and processes incoming nutrients. But it has limited glycogen capacity, and when energy repeatedly arrives faster than it’s being used, the liver has to deal with the overflow. That’s one reason chronically high energy intake combined with low demand can push the system toward greater fat storage compared to more active people.
Adipose tissue is the long-term storage site. It’s designed for it – from a survival perspective, storing extra energy as fat is the safest, most compact, and most reliable option.
This is why calories alone can feel like an incomplete explanation for many. It’s not only how much energy arrives, but how much capacity the body has to direct that energy into muscle glycogen and immediate use rather than long-term storage.
Hormone Control
Hormones are the master control system that coordinates all of this. The most important one in the fed state is insulin.
Insulin rises after eating, mostly after carbohydrates, but also after protein and fat to less degrees — and its job is to move nutrients out of the bloodstream and into tissues. It supports glycogen storage and fat storage, and it suppresses the release of fat from adipose tissue while it’s elevated.
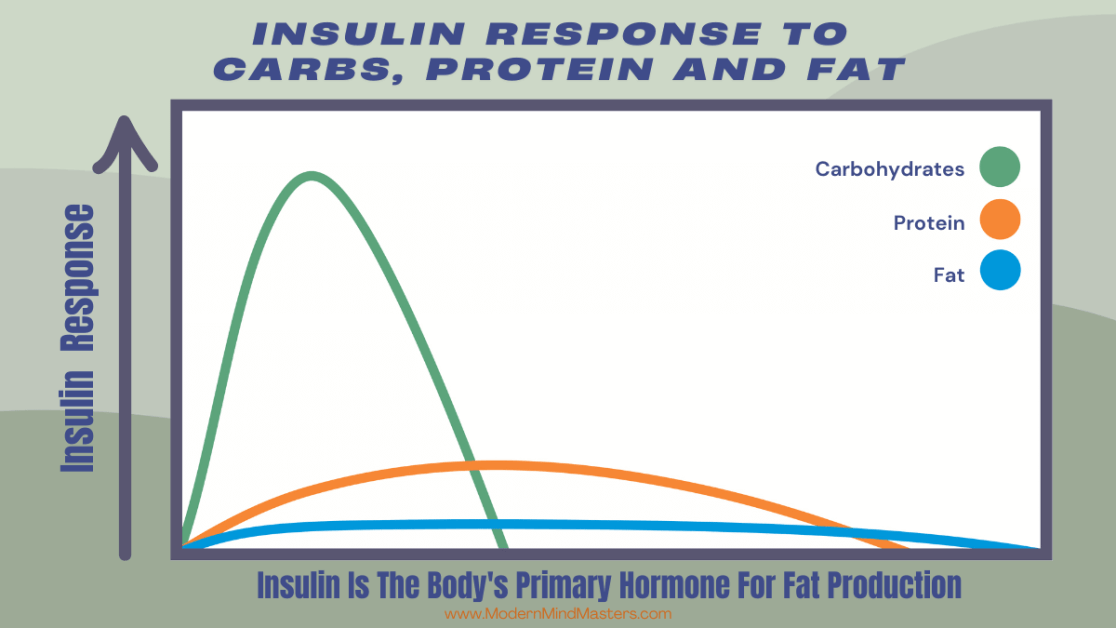
But it helps to understand why the body is so aggressive about handling glucose. It’s not because glucose is inherently a “better” fuel, contrary to most advice. It’s because glucose in the bloodstream has to be tightly controlled.
When glucose stays elevated in the bloodstream, it starts reacting with proteins and fats in a slow “sugaring” process called glycation, creating advanced glycation end products (AGEs) that stiffen and damage tissues and blood vessels. High glucose also increases oxidative stress and inflammation inside cells, which is a big part of why chronically elevated blood sugar raises the risk of vascular and nerve damage over time.
This is why insulin resistance and diabetes are so serious: when the body can’t clear glucose efficiently, glucose stays high for longer, and that increases damage risk through mechanisms like glycation and oxidative stress.
So insulin is neither a heroic nor a villainous hormone. It’s a blood-sugar control hormone, required for cell health, that also happens to be central to storage decisions.
On the other side are counter-regulatory hormones, especially glucagon and catecholamines (adrenaline/noradrenaline). These rise when food isn’t coming in or when energy demand spikes (like during exercise). They help mobilize stored fuels, including releasing fatty acids from adipose tissue.
Another common myth is that insulin is like an on/off switch, either burning glucose or not (i.e. burning fat). Fat release and fat burning don’t require insulin to be zero. They require insulin to be low enough, long enough, relative to the mobilization signals the body is receiving.
Fed vs Fasted Rhythm Across 24 Hours
Once you zoom out to a full day, the system becomes easier to understand.
After meals, insulin rises and the body prioritizes clearing glucose from the blood, using incoming fuel, and replenishing glycogen. During that time, fat release is reduced and some storage is normal.
Between meals and overnight, insulin falls, mobilization signals become more dominant, and the body increases access to stored fuel — especially fatty acids. This is why it’s completely possible to burn fat on a higher-carb diet: fat burning is often concentrated between meals, overnight, and around exercise, even if glucose is being prioritized right after meals.
So the real question isn’t “am I storing or burning?” The real question is whether your lifestyle creates a normal rhythm of fuel use, glycogen depletion, and access to stored fat, or whether you’re stuck in a pattern that keeps the body in a prolonged fed state with low demand for stored fuel.
That sets up the next part of the article, because modern life tends to increase the storage signals (frequent eating, processed foods, poor sleep, stress) while reducing the demand signals (low movement and low muscle use).
Can You Burn Fat While Eating Carbs?
There is much controversy these days surrounding carbohydrates. Mainstream narratives suggest they are essential for a balanced diet, while modern independent advice is trending toward low-carbohydrate diets such as the ketogenic or carnivore diet.
What both sides tend to bypass is context. Context is crucial and differs, sometimes significantly from person to person. While an athlete can consume hundreds of grams of carbs a day (and thrive), this same amount can (and often does) lead to diabetes over time in many, often with fatal results.
For those interested in exploring this idea in more detail, see this article here.
But to answer the question: Yes, you can burn body fat on a higher-carb diet, and people do it all the time. The confusion comes from a half-true idea: insulin reduces fat release, so people assume carbs “shut off” fat burning completely. In reality, your metabolism isn’t a binary switch. It’s a moving blend of fuels that shifts across the day depending on insulin level, time since last meal, and energy demand.
Insulin is Not an On/Off Switch
Insulin does act like a brake on fat release from fat tissue (lipolysis). But it’s not a locked door—it’s more like a dimmer switch.
After a carb-containing meal, insulin rises to do an urgent job: clear glucose from the blood and move it into tissues. While insulin is elevated, your body tends to prioritize burning more glucose and temporarily burning less fat. That’s normal physiology.
But insulin doesn’t stay high forever (unless someone is eating constantly, or has severe insulin resistance). As time passes after a meal, insulin falls. As it falls, the brake on fat release eases, fatty acids can be released again, and fat oxidation increases. So the relevant question isn’t “did I eat carbs?” It’s:
How much of your day is spent in a state where insulin is low enough for stored fat to be readily accessed?
This way of thinking aligns with how the body actually works, and is the key to orientating your daily meals and activity to better promote fat loss.
Fat Burning on Higher-Carb Diets
On a higher-carb diet, fat burning tends to be concentrated in predictable windows, typically between meals (especially if there are several hours between them), overnight during the longest stretch without food, and during and after exercise, depending on intensity and training status.
This is why “carbs prevent fat burning” is misleading. Carbs often shift you toward burning more glucose right after eating, but fat burning comes back online later when insulin drops and the body needs to cover energy demand from stored fuel.
Where people get stuck is when those windows disappear—usually from frequent snacking, liquid calories, or grazing. If you keep re-introducing glucose every hour or two, insulin may never fall much, and the body spends less time tapping stored fat. Fat burning still happens, but it’s compressed into a smaller part of the day (often mostly overnight).
Stepping back, carbohydrates are just one variable in the system. They can change when you burn fat across the day by shifting insulin and fuel use after meals, but they don’t rewrite the long-term accounting.
Over weeks and months, net fat loss still requires a sustained energy deficit—more energy leaving the system than entering it. Macronutrients influence appetite, cravings, training output, and how easy that deficit is to maintain, but they don’t determine fat loss in the absence of an energy deficit.
How Exercise Changes Fat Oxidation
Exercise is the clearest example that carbs don’t block fat burning. When energy demand rises, the body pulls from multiple fuel sources, and fat oxidation increases during lower-intensity work and especially between meals and overnight. Training also increases muscle glycogen turnover, creating more room to store glucose in muscle instead of pushing energy toward long-term storage. So even on higher carbs, regular activity expands the time and capacity for stored fat to be used.
In real life, this shows up as a simple contrast: some sedentary people maintain excess body fat even on 1,500 calories, while endurance athletes can eat double that (and often more) and remain lean. The difference isn’t genetics or luck—it’s energy demand and how much fuel the body is turning over each day.
Why is Fat Gain so Common Now?
If fat storage is normal biology, the obvious next question is why it has become such a widespread problem. The answer isn’t that humans suddenly became weaker or less disciplined. It’s that the environment changed in ways that constantly push the body toward higher intake, more frequent feeding, and lower fuel demand—all of which bias the system toward storage.
Ultra-Processed Foods and Overeating
Ultra-processed foods aren’t just tasty – they’re engineered to be easy to overconsume and are highly palatable, energy-dense, and quick to eat. Where our ancestors had natural limits as to how much they could consume in one sitting (think meatier foods that take longer to eat, not liquid milkshakes that can disappear in seconds), ultra-processed foods remove those speed limits through clever albeit slightly sinister food engineering.
A big part of the issue is the brain’s reward system. When you eat something that combines sugar/starch + fat + salt with strong flavors and a soft texture, it reliably produces a strong reward response.
Dopamine is involved here, not necessarily as a pleasure chemical, but as a learning and motivation signal. It reinforces the behavior and teaches the brain: this is worth seeking again. Over time, the brain becomes more sensitive to cues (seeing it, smelling it, stress, time of day), which can trigger cravings and snacking even when you’re not physically hungry.
Ultra-processed foods also tend to deliver a lot of calories with relatively weak satiety signals. They’re often low in protein and fiber, easy to eat quickly, and designed to keep the sensory experience high from the first bite to the last. The result is what researchers call passive overeating—not bingeing, not a failure of discipline, but consistently eating more than you intended because the food environment makes it effortless. I suspect this, combined with a lack of movement, is truly the cause of the modern obesity endemic.
You can feel this in real life. Most people could eat a huge plate of pasta—easily 2,000 calories once you include sauce, oil, and cheese—without it feeling outrageous in the moment. But try eating 2,000 calories of protein and fat from whole foods (steak, eggs, Greek yogurt, etc.) and it’s a completely different experience. It’s slower to eat, far more filling, and your appetite shuts it down sooner. That difference isn’t willpower—it’s food design, energy density, and satiety signals.

Frequent Eating and Refined Carbs
On paper, eating “little and often” sounds harmless. I followed it for years as a wannabe bodybuilder who struggled to get big meals down. But biologically, constant feeding changes the metabolic rhythm your body is designed to run on.
Every time you eat—especially carbohydrates—you trigger a fed-state response. Blood glucose rises, insulin rises, and the body shifts into storage and clearance mode. That’s not because glucose is a “better” fuel. It’s because glucose needs to be tightly controlled: when it stays elevated in the bloodstream for too long, it increases cellular stress through processes like glycation and oxidative damage. So insulin’s job is urgent—move glucose into tissues and bring blood levels back down.
The problem is what happens when you do that all day long. If you’re eating every couple of hours, you’re repeatedly layering fed-state signals on top of each other. Insulin may not stay sky-high, but it stays elevated often enough that the body spends less time in the between-meal state where it naturally increases access to stored fuel. In other words, the body isn’t “blocked” from burning fat—but the windows where fat release is easy and dominant become smaller and less frequent.
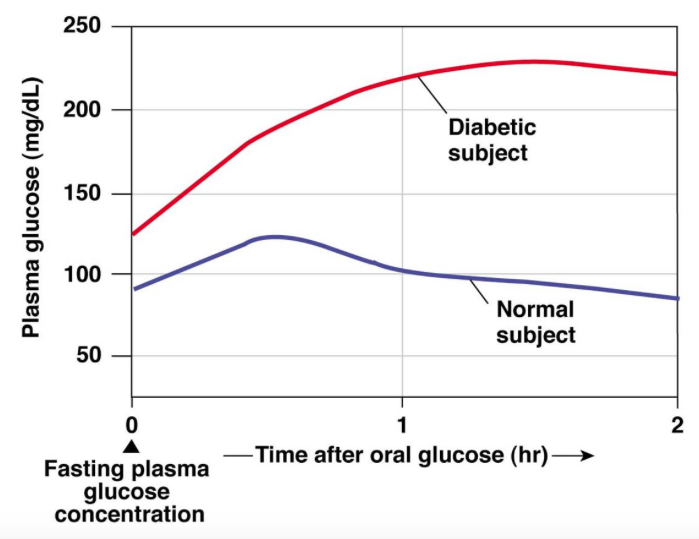
Refined carbohydrates make this worse because they’re absorbed quickly. They deliver glucose fast, which pushes a sharper insulin response, especially in people who are already insulin resistant. For those individuals, glucose can stay elevated longer, insulin stays elevated longer, and the return to baseline is slower. That creates the classic cycle: a spike, a drop, and then hunger arriving sooner than it should—often interpreted as “I need another snack,” when it’s really a fuel-regulation swing.
This isn’t an argument that carbs are inherently bad. It’s an argument that constant intake of rapidly absorbed carbs, in a low-activity context, can keep the body in a prolonged clearance-and-storage pattern—reducing the time spent drawing on stored energy and making appetite harder to regulate.
Sleep and Stress Effects on Fat Loss
When sleep is short or poor, appetite regulation moves predictably toward “eat more.” Ghrelin (a hunger-promoting signal) tends to rise, while leptin (which helps signal energy sufficiency) tends to fall, so the brain reads the situation as “we need more food.” At the same time, sleep loss reduces activity in the prefrontal cortex (the part involved in restraint and planning) and increases reactivity in reward-related circuits, which makes highly palatable foods feel more compelling and harder to ignore.
Stress pushes in a similar direction through a different pathway. Chronic stress elevates cortisol, which increases the drive to seek quick, high-reward energy—especially sugar and refined carbs—because the body is preparing for perceived demand.
Cortisol also increases glucose output from the liver and can worsen insulin resistance over time, which can amplify blood-sugar swings and bring hunger back sooner. So when late nights or stressful weeks make eating feel harder to manage, that’s not a character issue; it’s a shift in the underlying signals controlling hunger, reward, and energy availability.
Over time, this combination does more than increase intake. It makes calorie restriction feel harsher because sleep loss and stress increase subjective hunger, increase cravings, and reduce the brain’s ability to “hold the line” consistently. That’s why people often do fine for a few days, then rebound—because physiology is pushing them toward compensation.
Low Activity Reduces Muscle Fuel Demand
Modern life also reduces energy demand in a way that matters beyond “calories burned.” When muscle is used regularly, it becomes a major sink for glucose and a major site of fuel oxidation. When muscle isn’t used much, that sink shrinks.
This is one of the most underappreciated reasons fat gain has become common: it’s not only that people eat more, in both quantity and frequency—it’s that the body has fewer places to send incoming energy other than storage. Less movement means less glycogen turnover, less demand for fuel, and less metabolic “pull” from muscle. That makes it easier for excess energy to be stored and harder for stored energy to be accessed.
Can Fat Loss Slow Down or Stall?
Fat loss often slows for a simple reason: the body is adaptive. As you lose weight, the “cost” of running your body decreases, and your physiology makes small adjustments that make continued loss less automatic than it was at the start.
The first piece is lower energy expenditure. Some of this is just math: a lighter body burns fewer calories. On top of that, the body often adds a modest efficiency shift called adaptive thermogenesis—a small downshift in energy use that tends to show up during sustained dieting.
Importantly, this effect is usually not dramatic. For a typical sedentary middle-aged woman maintaining around ~1,800 calories/day, the adaptation is often on the order of roughly 50–200 calories/day, which is about 3–11% of daily burn. That’s enough to slow progress or create a plateau if nothing changes, but it’s not a “metabolism is broken” situation.
At the same time, appetite signals intensify. As fat mass drops, leptin tends to fall and ghrelin often rises, which makes hunger louder and food more compelling. This is one reason people feel like dieting gets harder over time: the body is nudging intake up while nudging expenditure down.
Then there’s the scale itself. A stall on the scale isn’t always a stall in fat loss because body weight includes water and glycogen, not just fat. Changes in carbohydrates, salt, sleep, stress, and training-related inflammation can temporarily increase water weight and hide fat loss for days—or even a couple of weeks—leading people to change plans too early.
Finally, if someone has insulin resistance and reduced metabolic flexibility, the process can feel less smooth. It may take longer after meals for insulin and glucose to settle, energy can feel less stable, and hunger can return sooner. That doesn’t prevent fat loss, but it can make consistency harder and plateaus more common if the person is relying on willpower rather than improving the signals.
What Should you Focus on to Make Fat Loss Easier?
Once you understand fat storage as a normal biological response, the goal stops being “try harder” and becomes “set the conditions that make fat loss easier to sustain.” You’re not looking for hacks, but leverage—changes that reduce hunger, increase fuel demand, and make progress measurable without obsession.
Improve Satiety (Increase Protein and Fat)
If there’s one principle that consistently makes fat loss easier, it’s this: eat in a way that naturally turns appetite down. Protein is the most reliable tool here because it increases fullness and tends to reduce cravings later. Whole foods help because they come with volume and slower eating speed—so you feel satisfied at a lower calorie load without feeling deprived.
I believe that this is one of the key reasons why the ketogenic diet is currently one of the most successful ways to promote fat loss. Not because there’s any magic in not eating carbs, but simply because it’s incredibly difficult to overeat protein and fat. Again, nature has hard limits on the speed of consumption of these natural whole foods.
Building muscle can also raise resting metabolic rate slightly, but the bigger advantage is what active muscle does to fuel handling: it soaks up glucose, improves insulin sensitivity, and increases how much energy you turn over each day.
The practical idea isn’t complicated: build meals around a solid protein anchor and keep most of your intake in foods that look like food. When people do that, they often find that “calories” become less of a daily battle because hunger stops shouting.
Reduce Appetite Drivers (Sleep, Stress, Environment)
For most people, fat loss doesn’t fail because they don’t know what to do. It fails because their appetite keeps dragging them back to old patterns. Poor sleep, chronic stress, and a house full of “easy calories” all push in the same direction: you feel hungrier, cravings hit harder, and it takes more effort to stay on track.
Start with sleep, because it quietly controls everything else. When you’re underslept, food is more tempting and “reasonable” decisions are harder to hold all day. Stress does something similar—especially when the easiest comfort foods are always within reach.
That last part matters more than people like to admit: your environment usually beats your willpower. If there are foods you repeatedly overeat, keeping them in the house is basically agreeing to fight the same battle every night. The most effective change is often the simplest one: remove the trigger foods, or make them inconvenient, and make the default options the ones that support your goal.
Track Better Metrics
Finally, measure in a way that matches biology. Day-to-day scale weight is noisy because water and glycogen fluctuate, especially for women with monthly cycles. What matters is the trend.
A weekly average weight, combined with waist measurement and a simple performance marker (strength, steps, or training consistency), gives you a much clearer signal. If weight is flat but waist is shrinking and strength is steady, you’re still moving in the right direction. Better tracking prevents the most common mistake: changing a plan that’s working because the scale temporarily stalled.
Final Thoughts
The most important takeaway is that your metabolism isn’t some mysterious force you’re “stuck with.” It’s a responsive system. It adapts to what you repeatedly do—how often you eat, what you eat, how much you move, how you sleep, and how much stress you carry. When you understand the rules it’s following, you can stop fighting it and start getting it to work with you.
Fat loss is really about creating the conditions where stored energy is used consistently. That means keeping appetite manageable, keeping muscle demand high, and avoiding patterns that keep you in a constant fed state with low fuel turnover. Over time, the outcome still comes down to energy balance—but the ease of maintaining that balance is where most people win or lose.
So focus on the levers that make metabolism work in your favor:
- Build meals around protein and mostly whole foods so hunger stays quiet.
- Lift weights and move daily to increase fuel demand and improve partitioning.
- Protect sleep, reduce chronic stress, and remove the foods that reliably derail you.
- Track the trend (weekly averages, waist, strength) so normal scale noise doesn’t knock you off course.
Done consistently, this stops being a guessing game. You’re not trying to “beat” your metabolism—you’re learning how to run it well.
FAQs
Can you burn fat while eating carbs?
Yes. After a carb-containing meal, insulin rises to clear glucose from the blood, so the body burns more glucose and temporarily burns less fat. As insulin falls between meals and overnight, fat release increases again and stored fat is used. On higher-carb diets, most fat burning happens between meals, overnight, and around exercise. The pattern that reduces these “fat-access windows” is frequent snacking or sipping calories all day, which keeps insulin elevated more often.
If insulin is high, does that mean fat burning stops?
No. Insulin suppresses fat release from adipose tissue, but it acts more like a dimmer switch than an on/off button. Higher insulin generally means less fat is released in that moment, but fat use doesn’t go to zero. The bigger issue is time: if insulin stays elevated for long periods (frequent refined carbs, grazing, insulin resistance), the body spends more time prioritizing glucose disposal and less time accessing stored fat comfortably. Improving insulin sensitivity shortens how long glucose and insulin stay elevated after meals.
How can you maximise fat loss and avoid plateaus?
Focus on the variables that make an energy deficit easier to sustain. Keep protein high and most foods minimally processed to control hunger. Maintain or build muscle with resistance training and keep daily movement high to preserve fuel demand. Protect sleep and reduce chronic stress so appetite signals don’t work against you. Track progress using weekly weight averages and waist measurements, not single weigh-ins, and make small adjustments only after consistent trends—not short-term fluctuations.